
Millions of patients had non-urgent operations cancelled during the Covid-19 pandemic as the NHS came "close to collapse", a major public inquiry has concluded. The latest report from the UK Covid-19 Public Inquiry lays bare the scale of disruption across the health service, revealing how both Covid and non-Covid patients suffered as hospitals struggled to cope.
Inquiry chairwoman Baroness Heather Hallett said the system was pushed to its limits, with some patients failing to receive the care they would normally expect. She added: "Some people were not admitted to hospital when they should have been. Those taken to hospital in an ambulance often waited hours to be admitted, putting them and the ambulance crews at risk. Healthcare staff had to be redeployed to the front line, leaving other aspects of care at risk. Staff-to-patient ratios were diluted, the supply of medical equipment was a significant concern and some patients were not admitted to intensive care units despite their serious condition."
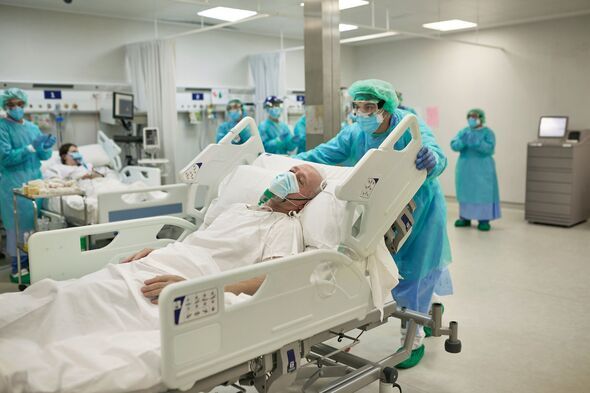
She highlighted how "fragility" in the NHS had "profound consequences" when the pandemic hit, as she listed a number of steps taken to prevent the spread of the virus.
These included the pausing of elective (non-urgent) treatment in spring 2020.
"Across the UK, millions of people had non-urgent operations cancelled," she said.
"For many, it was devastating to learn that their long-awaited operation was going to be further delayed - to give one example: people waiting for hip replacements had to live in constant pain with decreased mobility.
"For some, their condition deteriorated to such an extent that surgery was no longer an option."
And she highlighted the "high cost" of pausing bowel cancer screening in Scotland, Wales and Northern Irlenad, adding: "The lack of screening for colorectal cancer, for example, led to missed and late diagnoses, longer waits for colorectal cancer treatment and ultimately loss of life."
Lady Hallett said: "The fact that the treatment of patients for life-threatening and life-changing conditions had to be postponed indicates the extreme pressure on the system.
"Desperate measures had to be taken to ensure people who needed treatment for Covid-19 could be cared for and that healthcare systems did not collapse entirely."
Meanwhile, Lady Hallett spoke of the "harmful consequences" of visiting restrictions in hospitals as she said that visits for dying patients should be "facilitated as far as possible".
Her new report lays bare the "devastating impact" of restrictions which led to many dying alone.
Visiting restrictions became some of the "most contentious" measures taken to reduce the spread of the virus and led to "deeply distressing" experiences for patients, family and friends.
The probe found that while restrictions "may be unavoidable" in a pandemic, visits for dying patients should be suspended "for the shortest time possible" and that alternative ways of making contact should be provided.
Lady Hallett said: "Restrictions meant that many patients died without the comfort of being surrounded by their loved ones and were deprived of the opportunity to say goodbye.
"This has had a devastating impact on bereaved family members."
Bereaved families told of saying goodbye to their loved ones over text message, while health workers recalled helping dying patients video-call their crying families.
Sam Smith-Higgins, part of Covid-19 Bereaved Families for Justice Cymru, said of her father: "I received a call from the doctor who told us that he had deteriorated and that he was dying.
"To not be able to be with my father and to hear that news was completely devastating.
"He was with a nurse and so I was constrained to saying my farewell to my father by text message, with the hope that it would be read out to him.
"It is truly difficult to put into words how painful it is to say farewell to a loved one by text message."
Margaret Waterton, of Scottish Covid Bereaved, said: "When I was with mum, I would talk with her and hold her hand. I could not hug her as I was not allowed to.
"Wearing full PPE, all that mum could see of my face were my eyes. I had to make sure that I spoke as clearly as possible through the mask and visor.
"Holding hands when wearing double gloves is far from the skin-to-skin contact that is so comforting.
"Those would be the last things my mum would see, me dressed in full PPE, not able to hug her or kiss her or properly hold her hand."
Another bereaved family member, who was not named, told the inquiry's listening exercise, Every Story Matters: "I didn't want dad to go into hospital, my dad didn't want to go into hospital either... he loved being at home, if he's going to die, he wanted to die at home.
"We knew if he went into hospital, I would wave goodbye at the door and the chances are I would never see him again and he would die alone in hospital."
The restrictions, which were seen as a "necessary step" to reduce spread, meant an "additional burden" fell on healthcare workers to provide dying patients with the comfort they were missing, the chairwoman found.
Patricia Temple, a nurse on a cardiac care unit from March to November 2020, told the inquiry of the time she heard a patient with learning difficulties asking his mother over the phone to come and see him and not understanding why she could not visit.
Professor Kevin Fong, national clinical adviser in emergency preparedness, resilience and response for Covid-19 to NHS England during the pandemic, relayed an account from one health worker who said: "Showing someone their family member dying, on an iPad was awful, that's what I can't get out of my head.
"The family are crying and I'm holding the iPad and crying. For me it was too much."
Gillian Higgins, a member of Covid-19 Airborne Transmission Alliance, said she saw a "huge number of patients dying" when she worked in the intensive care unit (ICU).
"It was usual to arrive for a... shift only to become aware that none of the patients from my previous shift were still there; and for it to transpire that none of them had survived.
"I did not see any patients recover and be discharged from Covid-19 ICU during my shifts working there. It had become commonplace to see body bags containing people that had died being moved around the hospital to the mortuary."
Visiting restrictions also left vulnerable patients without "vital support" at appointments or when they were receiving care, Lady Hallett found.
She highlighted the impact on pregnant women and patients with dementia and learning disabilities in particular.
It comes as the Government announced plans to give people stronger rights for hospital and care home visits.
Changes in the law were initially proposed in 2023 by the former Conservative government.
The Government said it will "distribute comprehensive guidance and resources to make visitation rights clear".
The Department of Health and Social Care said ministers are "exploring bringing forward proposals for legislating visiting rights as part of wider reform work".
The guidance will make clear that patients and residents in care homes, hospitals and hospices "will no longer be cut off from their loved ones unless in exceptional circumstances", the department said.