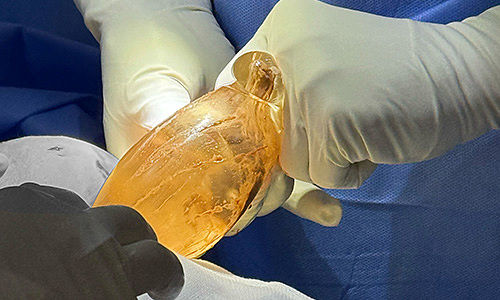
In selected cases, patients may not require postoperative analgesics or antibiotics, except in situations such as Baker grade IV capsular contracture or seroma within the implant pocket. Discharge may be considered approximately four hours after surgery, depending on clinical evaluation.
In some cases, textured breast implants manufactured using salt-loss techniques may be more difficult to assess for rupture using ultrasound. Patients with textured implants, including those from brands such as Allergan, Polytech, or Eurosilicone, are typically advised to provide information about the implant type to support clinical assessment of implant integrity, including folding, leakage, or rupture.
In addition to implant evaluation, clinical assessment may include monitoring of breast tissue, implant- conditions, the fibrous capsule, and the implant pocket, as well as screening for malignancy and other abnormalities such as rupture, folding, or seroma.
|
Motiva breast implant rupture 2 years after augmentation. Photo courtesy of Dr. Cao Vu |
MSc, MD Ho Cao Vu has identified several factors associated with early breast implant rupture.
According to Dr. Vu, in inframammary fold (IMF) or periareolar breast augmentation, the use of an incision that is relatively small compared to the implant size, particularly implants with large diameter or high projection, may increase the risk of implant damage during insertion, potentially affecting long-term durability.
In addition, implant pocket revision performed using blunt dissection while the muscle is pharmacologically relaxed may lead to discrepancies in pocket assessment once muscle tone returns. This may result in insufficient pocket dimensions, particularly along the medial border and base circumference, contributing to implant compression or folding at the lower pole.
In transaxillary breast augmentation using blunt dissection, early implant rupture has been associated with two primary factors: insufficient pocket creation, which may prevent even implant distribution, and the use of instruments to revise the pocket after implant placement, which may introduce mechanical stress.
Incorrect placement between anatomical planes may subject the implant to compressive forces from the pectoralis major muscle. In such cases, the superomedial quadrant (upper inner quarter) is often exposed to the highest pressure.
Early implant rupture has also been observed in patients with a short nipple-to-inframammary fold distance. In these cases, pocket creation may be biased toward the upper pole, leading to superior displacement of the implant and increased pressure from the pectoralis major muscle, particularly during positions or activities that increase muscle tension. Over time, uneven pressure distribution may increase the risk of implant damage.
Clinical signs suggestive of an insufficient implant pocket in patients with a short nipple-to-inframammary fold distance (preoperative measurement <5 cm) may include upper pole fullness, limited fullness at the lateral and lower poles, and a downward nipple orientation distinct from breast ptosis.
Early breast implant rupture may also occur when implant size is not well matched to the patient’s anatomical characteristics. In such cases, explantation may be required within several years postoperatively, with some reported instances occurring earlier.
The following section summarizes observations from Dr. Vu regarding causes, clinical signs, and management of ruptured breast implants.
|
Breast implant rupture 5 years after augmentation. Photo courtesy of Dr. Cao Vu |
After placement, the posterior surface of the implant typically rests against the chest wall, while the anterior surface is covered by the pectoralis muscle, breast tissue, and skin. Factors such as inadequate pocket size, oversized implants, suboptimal positioning, persistent muscular pressure, and capsular contracture may contribute to early implant failure.
Potential indicators of suboptimal implant positioning may include:
– Progressive widening of the intermammary distance
– Gradual flattening of the upper pole, with increased distance from the upper pole to the nipple
– Excessive upper pole fullness associated with superior implant displacement
– Lateral displacement of the breast, particularly noticeable in the supine position
In some cases, early postoperative outcomes may appear satisfactory, while later complications develop over time.
One reported case involved a 36-year-old patient (45 kg, 157 cm) who underwent breast augmentation on Sept. 8, 2023. At a two-day postoperative follow-up, breast shape was reported as symmetrical and satisfactory. However, approximately two years later, on Dec. 18, 2025, ultrasound examination identified rupture of the left implant.
The patient reported intermittent sharp pain and changes in breast shape compared to the early postoperative period. Findings included implant bottoming out and increased visibility on the right side, and rupture on the left. According to Dr. Vu, this represented an early occurrence relative to typical timelines.
Explantation was recommended, followed by a waiting period of six months to one year to allow tissue stabilization before considering re-augmentation. A cautious, staged approach was advised to reduce the risk of recurrence.
Dr. Vu indicated that contributing factors in this case may have included suboptimal pocket creation, implant size relative to anatomical characteristics, and localized pressure within the implant pocket.
|
Rupture of textured Allergan breast implants 7 years after augmentation. Photo courtesy of Dr. Cao Vu |
Dr. Vu has also reported that long-standing implant rupture may lead to inflammatory responses between silicone gel and surrounding tissues within the implant pocket. Observations may include papillomatous changes, edema, and chronic inflammation. In cases involving capsular contracture, timing of reimplantation requires careful evaluation. Early explantation is generally recommended once rupture is identified.
Explantation using an ultrasonic scalpel with laryngeal mask anesthesia is described as a minimally invasive approach that may support shorter recovery times in selected patients.
The general procedural steps include:
Step 1: Assessment of the implant pocket, including bottoming out, lateral displacement, insufficient pocket dimensions, and pressure imbalance
Step 2: Administration of laryngeal mask anesthesia
Step 3: Dissection into the implant pocket using an ultrasonic scalpel
Step 4: Removal of the ruptured implant
Step 5: Cleaning of the implant pocket
Step 6: Evaluation of capsular contracture, fibrous bands, and pocket condition (over- or under-dissected)
For patients considering re-augmentation, the implant pocket is reassessed to determine appropriate pressure distribution. Techniques such as pocket expansion and capsulorrhaphy may be used to optimize conditions prior to placement of a new implant or in preparation for a future procedure.
The use of ultrasonic scalpel techniques in this context is associated with minimally invasive handling and may allow for relatively early return to daily activities, depending on individual recovery and clinical assessment.